Lymphoblastic lymphoma in children and teenagers
The information provided on www.fcarreras.org is intended to support, not replace, the relationship that exists between patients/visitors to this website and their physician.
Information endorsed by… ![]()
Information reviewed by Dr. Rocío Parody Porras, Doctor specialising in Haematology. Member of the Management of REDMO (Bone Marrow Donor Registry) and of the Foundation’s medical team. Barcelona Medical Association (Co. 35205)
What is lymphoblastic lymphoma in children and teenagers and who does it affect?
 Lymphoblastic lymphoma is a type of non-Hodgkin’s lymphoma that particularly affects children and adolescents. Lymphoblastic lymphoma affects around 25-30% of non-Hodgkin’s lymphomas in paediatric patients.
Lymphoblastic lymphoma is a type of non-Hodgkin’s lymphoma that particularly affects children and adolescents. Lymphoblastic lymphoma affects around 25-30% of non-Hodgkin’s lymphomas in paediatric patients.
The cancer cells of lymphoblastic lymphoma are very young lymphocytes called lymphoblasts. The affected cells are the same as in acute lymphoblastic leukaemia in children. In fact, if more than 25% of bone marrow is composed of lymphoblasts, the disease is classified and treated as acute lymphoblastic leukaemia as opposed to lymphoma. 80% presents as acute leukaemia and the rest affects the lymph nodes, bones and skin.
The majority of lymphoblastic lymphomas are developed in the T-cells and are called precursor T-cell lymphoblastic lymphomas. T-cell lymphoblastic lymphomas are most common in adolescents, young patients and males.
A small number of lymphoblastic lymphomas (10%) are developed in the B cells and are called precursor B-cell lymphoblastic lymphomas.
What are the causes of lymphoblastic lymphoma?
Research in this field is important and the genetic changes that occur in the affected cells are becoming known. However, the triggers or factors that have given rise to the lymphoma are unknown.
These begin when a white blood cell that fights infections, known as a lymphocyte, suffers a genetic mutation. The mutation tells the cell to multiply quickly, creating many diseased lymphocytes that continue to multiply. This produces too many diseased and ineffective lymphocytes in the lymph nodes and causes the lymph nodes, spleen and liver to swell.
Leukaemia and lymphomas, like other cancers, are not contagious. See section Leukaemia, bone marrow and blood cells.
What are the symptoms of lymphoblastic lymphoma?
T-cell lymphoblastic lymphoma often originates in the thymus and forms a mass behind the breastbone and in front of the windpipe. This can lead to breathing problems, which can be the first symptom of lymphoma in many patients. It can grow very quickly and therefore needs to be diagnosed and treated quickly.
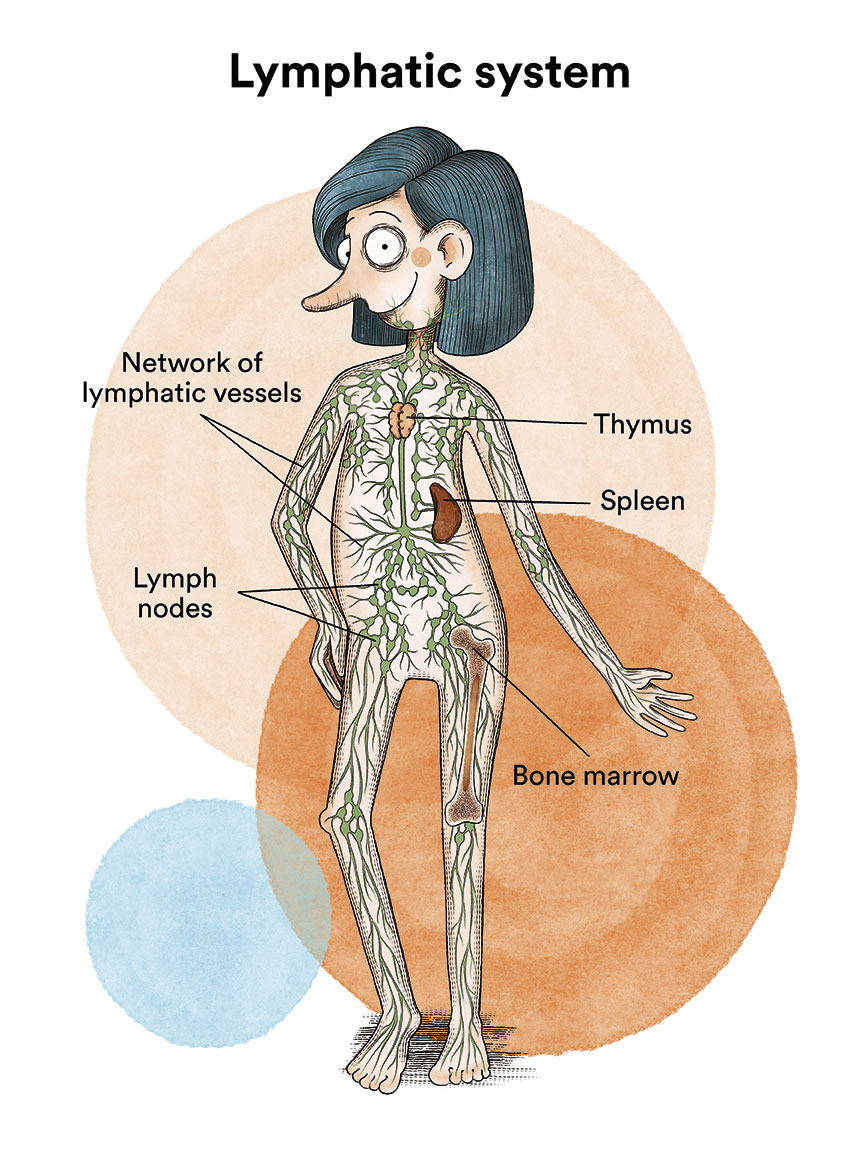
70% of patients may also present with affected and inflamed lymph nodes, especially in the clavicle, cervical spine and armpits. The bone marrow and nervous system may also be affected, although this is present in fewer patients.
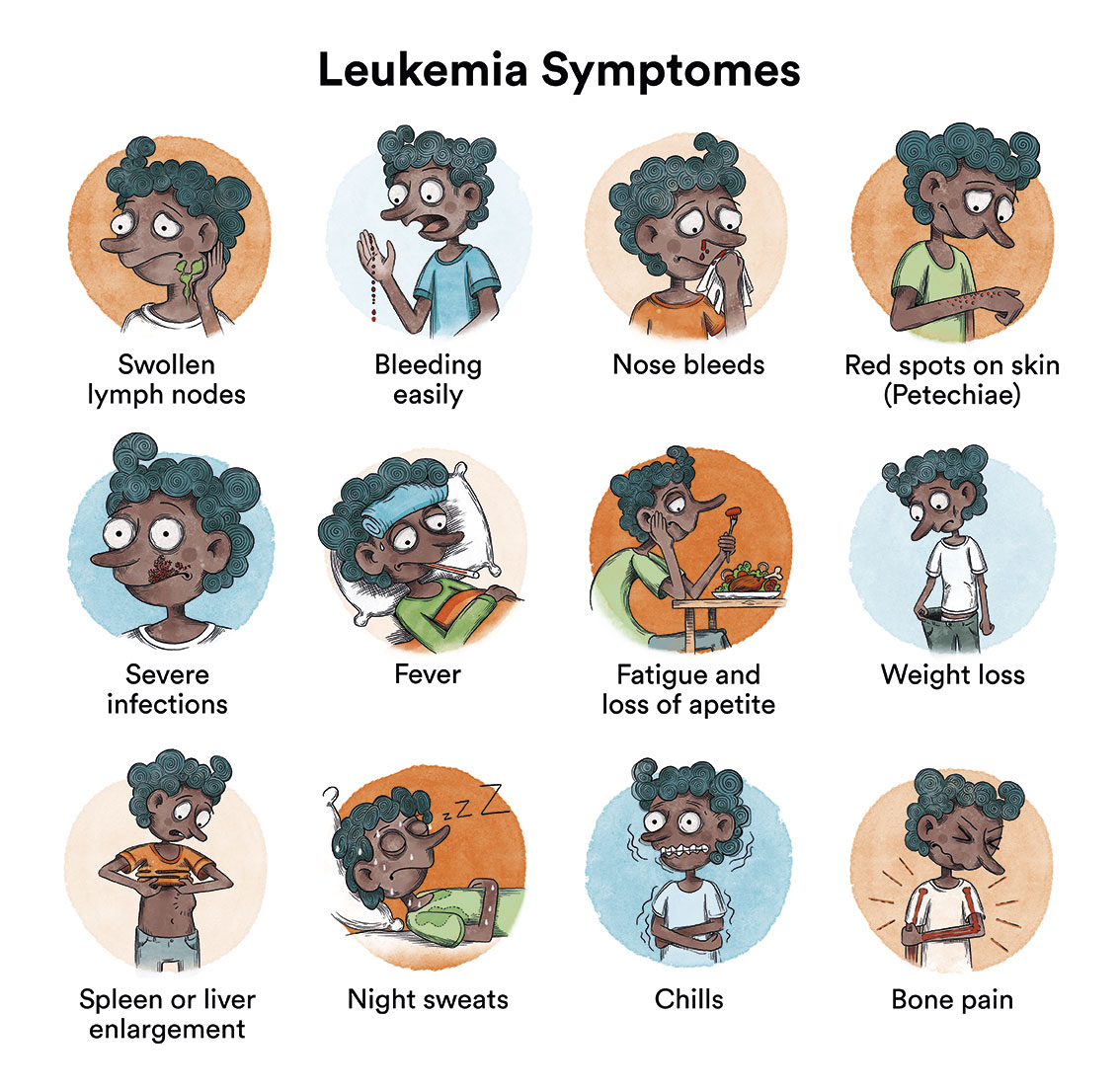
Not all children or adolescents with lymphoma present with the same symptoms. Other symptoms may include:
- Lumps in the neck, armpits, stomach, testicles or groin (sometimes called “swollen glands”)
- Fever
- Night sweats
- Fatigue
- Unexplained weight loss and/or loss of appetite
- Itchy skin
- Shortness of breath
- Cough
- Chest pain
- Swollen abdomen
How is lymphoblastic lymphoma diagnosed?
Generally, if a child presents the characteristic symptoms, a blood test will be undertaken. The doctor will also request a biopsy of the swollen lymph node in order to establish a diagnosis. During the biopsy, all or part of the abnormal lymph node will be extracted and observed under a microscope in a laboratory
The diagnosis is confirmed by a bone marrow puncture (iliac crests) and analysis of the cells obtained.
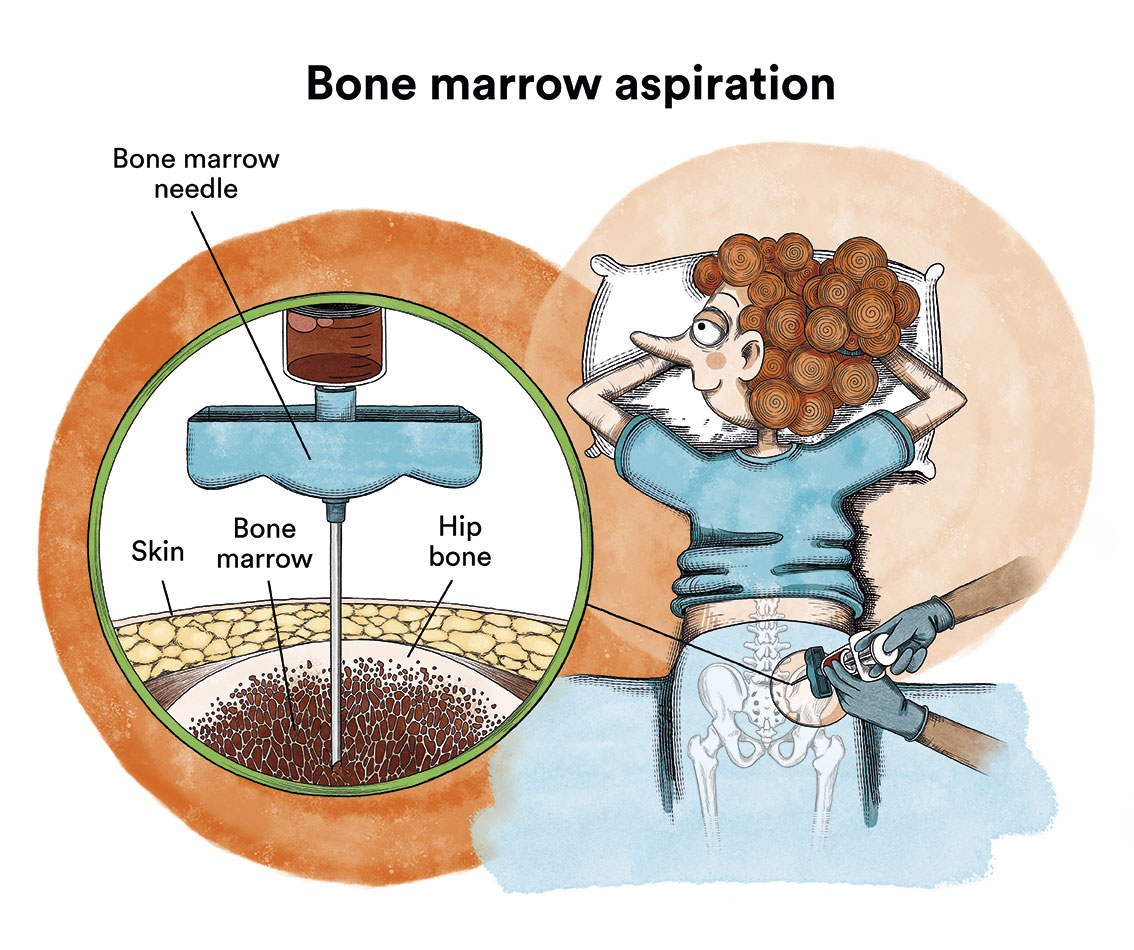
What is the treatment for lymphoblastic lymphoma?
Lymphoblastic lymphoma grows rapidly, but its prognosis has changed significantlysince patients have been treated with guidelines similar to those used in acute lymphoblastic leukaemia, with central nervous system prophylaxis.
Treatment is based on intensive chemotherapy and radiotherapy for central nervous system prophylaxis. Bone marrow transplant may be used in cases of relapsed disease.

What are the chances of children and teenagers with lymphoblastic lymphoma being cured?
Approximately 80% of children who undergo treatment are free of disease five years after diagnosis.
Links of interest concerning medical issues relating to lymphoblastic lymphoma in children and teenagers
Childhood Lymphoblastic Lymphoma. Dana Farber Cancer Institute
Types of Non-Hodgkin Lymphoma in Children. American Cancer Society
Childhood Non-Hodgkin Lymphoma Treatment. National Cancer Institute
Lymphoma in Children. St Jude Children’s Research Hospital
Useful links: local entities (resources and services)
All these organisations are external to the Josep Carreras Foundation.
ANDALUCÍA
ARAGÓN
ASTURIAS
CASTILLA LA MANCHA
CASTILLA LEÓN
CATALUÑA
VALENCIAN COMMUNITY
EXTREMADURA
GALICIA
BALEARIC ISLANDS
CANARY ISLANDS
LA RIOJA
MADRID
- AAA (asociación de adolescentes y Adultos Jóvenes con Cáncer)
- ASION
- FUNDACIÓN CAICO
- FUNDACIÓN ALADINA
- FUNDACIÓN UNOENTRECIENMIL
MURCIA
NAVARRA
BASQUE COUNTRY
Support and assistance
We also invite you to follow us through our main social media (Facebook, Twitter and Instagram) where we often share testimonies of overcoming this disease.
If you live in Spain, you can also contact us by sending an e-mail to imparables@fcarreras.es so that we can help you get in touch with other people who have overcome this disease.
* In accordance with Law 34/2002 on Information Society Services and Electronic Commerce (LSSICE), the Josep Carreras Leukemia Foundation informs that all medical information available on www.fcarreras.org has been reviewed and accredited by Dr. Enric Carreras Pons, Member No. 9438, Barcelona, Doctor in Medicine and Surgery, Specialist in Internal Medicine, Specialist in Hematology and Hemotherapy and Senior Consultant of the Foundation; and by Dr. Rocío Parody Porras, Member No. 35205, Barcelona, Doctor in Medicine and Surgery, Specialist in Hematology and Hemotherapy and attached to the Medical Directorate of the Registry of Bone Marrow Donors (REDMO) of the Foundation).
Become a member of the cure for leukaemia!


