Childhood acute lymphoblastic leukaemia, type B
Leukaemia is the most common cancer among children. It affects more than 350 children a year in our country, a third of which are under 4 years of age. Leukaemia accounts for 30% of all paediatric cancers, with B-acute lymphoblastic leukaemia being the most common form among children (80% of cases)
The information provided on www.fcarreras.org is intended to support, not replace, the relationship that exists between patients/visitors to this website and their physician.
Leo
Acute Lymphoblastic Leukaemia.
“Leo was diagnosed with high-risk acute lymphoblastic leukemia when he was 3 years old. After a long time of treatment, we have finally returned home and Leo is great, just going to the hospital to check-ups. He also had a little brother, Noah. In addition to the importance of continuing researching and promoting bone marrow donation, the support between families is essential. We send you a lot of strength, unstoppable”.
Information endorsed by… ![]()
Information provided by Dr. Susana Rives. Specialist in Paediatric Haematology at the Sant Joan de Déu Hospital in Barcelona.
What is leukaemia, bone marrow and what are the types of blood cells?
Leukaemia is a type of blood cell and bone marrow cancer. See section Leukaemia, bone marrow and blood cells.
What is B-acute lymphoblastic leukaemia?
Acute lymphoblastic leukaemia (ALL) is a type of cancer in which the bone marrow produces too many immature lymphocytes (a type of white blood cell), known as lymphoblasts. These cells prevent the growth of other blood cells. Lymphocytes are a type of leukocyte or white blood cell and can be of two types, B and T. Depending on whether the lymphoblasts originate from B or T cells, ALL will be referred to as B- ALL or T- ALL. ALL is the most common type of cancer among children and most diagnoses are of B-acute lymphoblastic leukaemia (80% of leukaemia cases in children).
 As we have seen in ‘Leukaemia, bone marrow and blood cells’ , the bone marrow produces blood stem cells (immature cells) that will eventually develop into mature blood cells. A blood stem cell becomes a myeloid stem cell or a lymphoid stem cell.
As we have seen in ‘Leukaemia, bone marrow and blood cells’ , the bone marrow produces blood stem cells (immature cells) that will eventually develop into mature blood cells. A blood stem cell becomes a myeloid stem cell or a lymphoid stem cell.
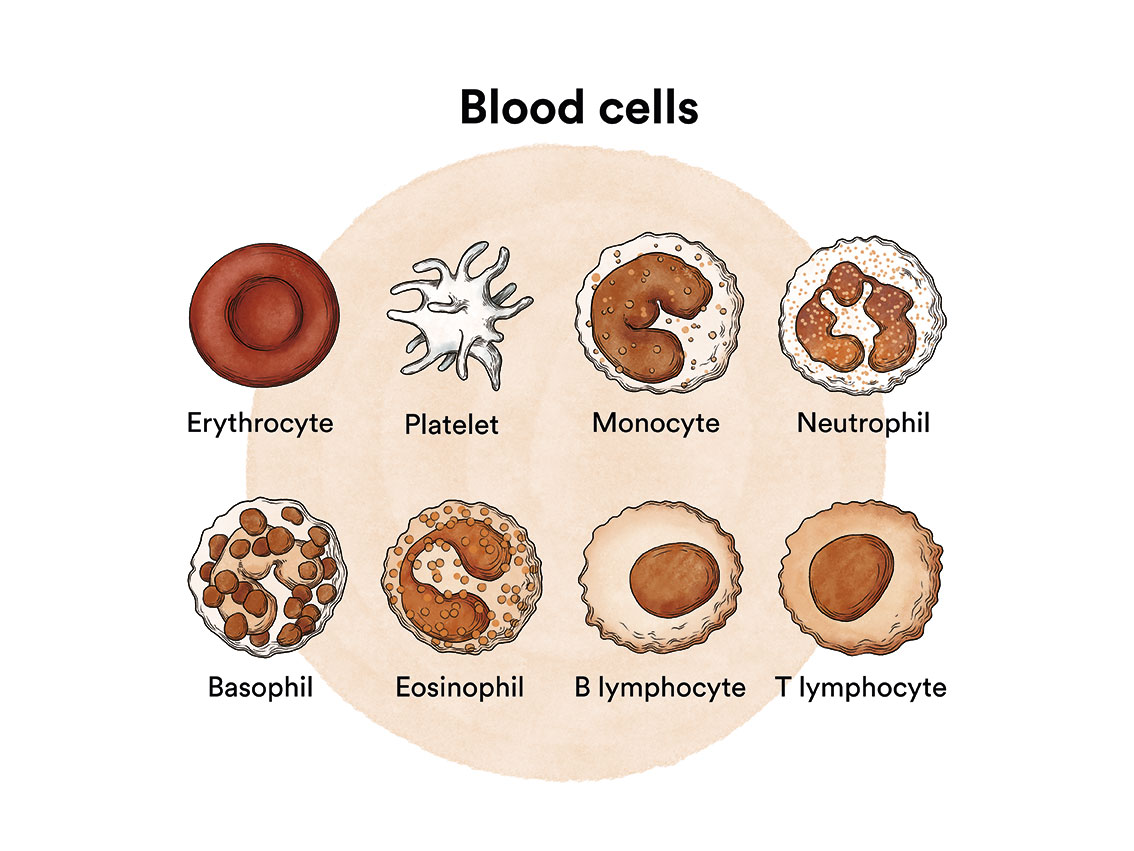
A myeloid stem cell develops into one of the three types of mature blood cells:
- Red blood cells, which carry oxygen to other tissues and organs in the body.
- Granulocytes, white blood cells that help fight infection and other diseases.
- Platelets, which help blood to clot when a blood vessel ruptures.
A lymphoid stem cell develops into a lymphoblast and later into one of the three types of lymphocytes (white blood cells):
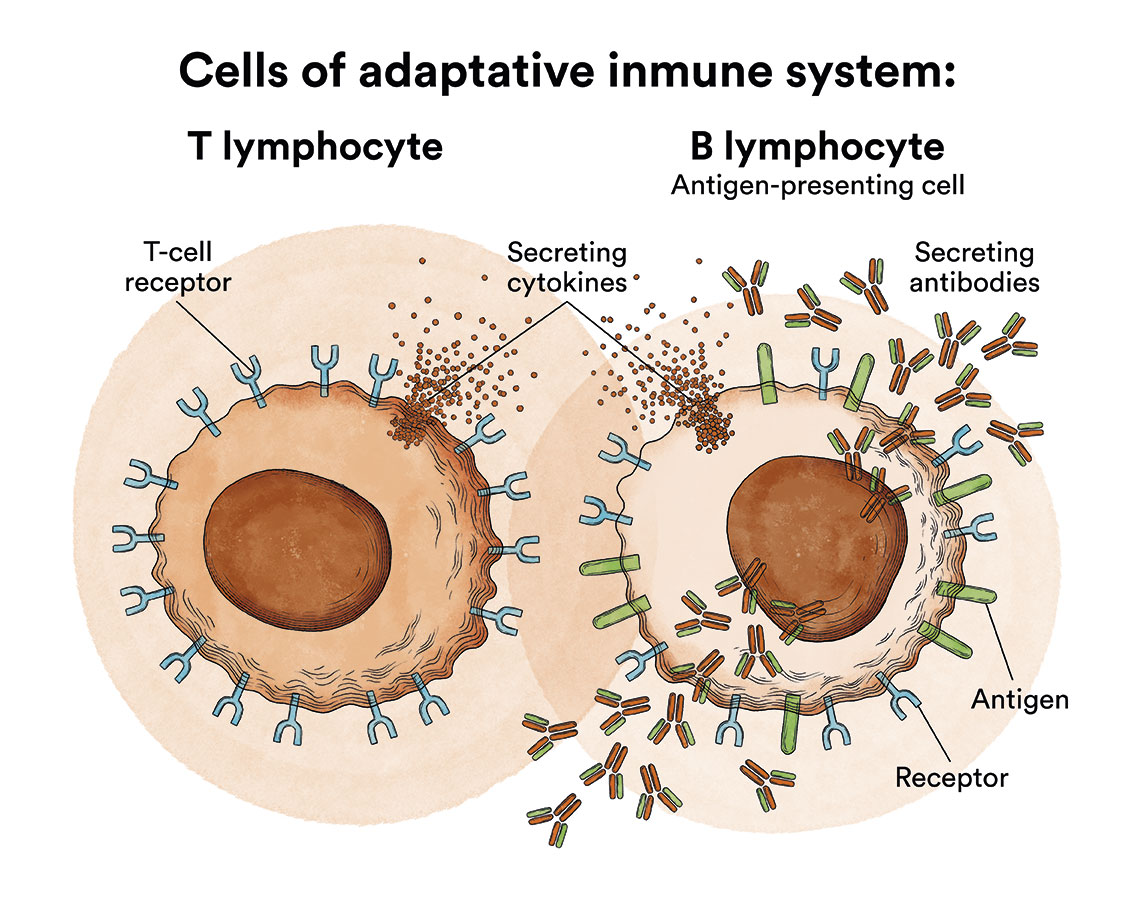
- B lymphocytes, which produce antibodies to help fight infections in the body.
- T lymphocytes, which help B lymphocytes produce antibodies to fight infection.
- Natural cytolytic lymphocytes or NK lymphocytes (natural killer), a type of immune cell that contains enzymes which can destroy tumour cells or virus-infected cells.
In children affected by B-acute lymphoblastic leukaemia, there are too many stem cells that transform into B lymphoblasts.
What are the causes of B-acute lymphoblastic leukaemia?
The exact cause of B-ALL is unknown. Research in this field is important and the genetic changes that occur in leukaemic cells are becoming known. However, in most children with B-ALL, the triggers or factors that led to the leukaemia are unknown.
In a minority of children there are some genetic diseases that predispose them to the development of acute lymphoblastic leukaemia. This is the case for children with Down syndrome or other syndromes such as Li-Fraumeni syndrome, ataxia-telangiectasia, Fanconi anaemia and others. Other factors that increase the likelihood of developing leukaemia may include exposure to radiation prior to birth (X-rays) or having received chemotherapy for another cancer.
Siblings of a child with leukaemia, compared to other children, have a small increased risk of developing leukaemia. However, this risk is very low, less than 1 per thousand.
Leukaemia, like other cancers, is not contagious. See section Leukaemia, bone marrow and blood cells.
What are the symptoms of B-acute lymphoblastic leukaemia?
In B-acute lymphoblastic leukaemia, the production of normal blood cells is disrupted by the growth of leukaemic cells in the bone marrow. This can lead to:
- Tiredness and paleness (due to anaemia).
- Appearance of purple and small pink patches on the skin (petechiae) or other bleeding due to low platelet count.
- Fever and infections that do not progress well (due to leukocyte malfunction).
- Joint and bone pain or lameness (due to leukaemia cells having invaded the bone marrow).
- Adenopathies or enlarged lymph nodes (due to the occupancy of leukaemic cells in the lymphatic system).
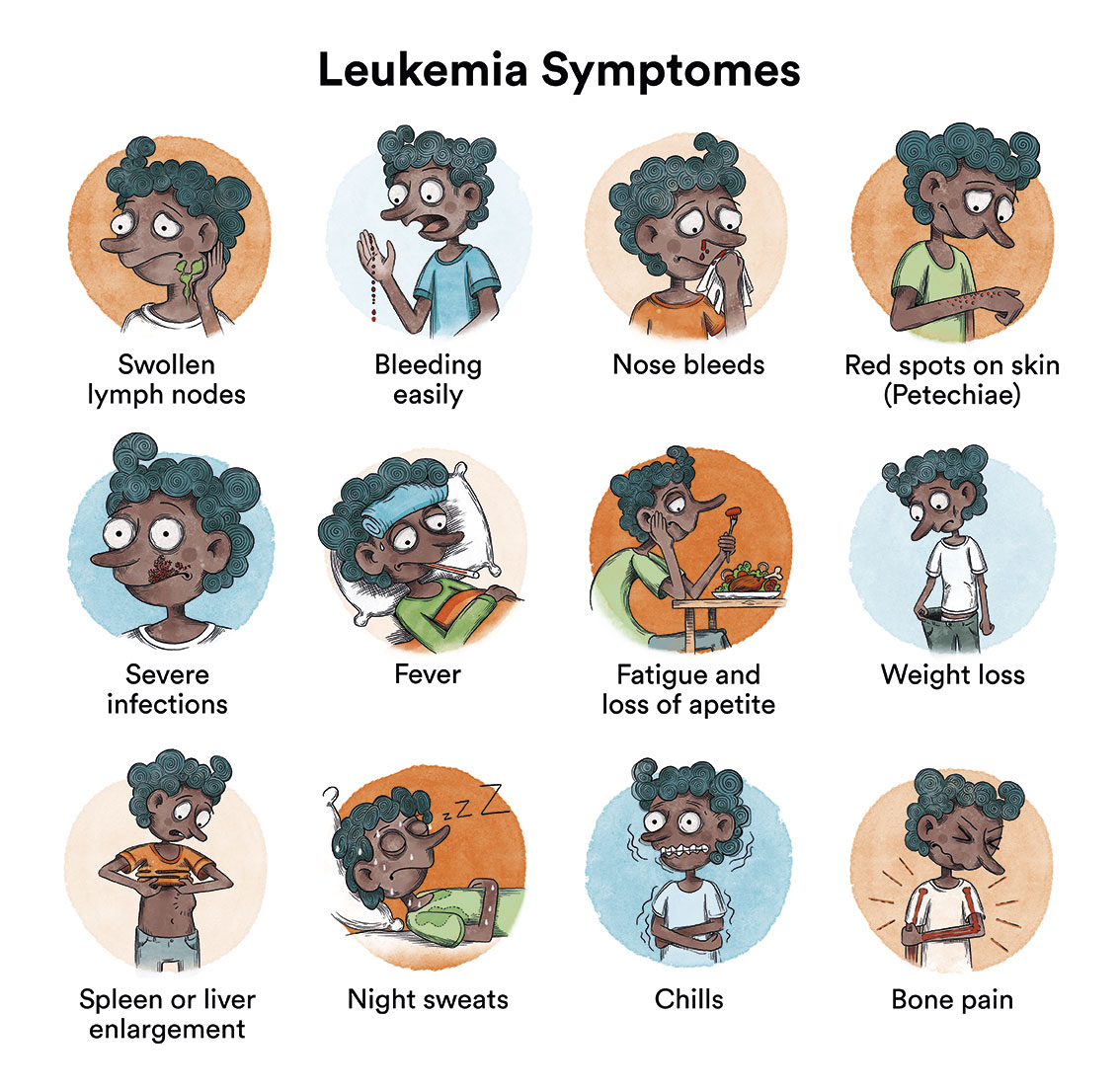
At the onset of the disease, all these symptoms can be very similar to those of a virus infection. When symptoms continue for more than 2-4 weeks, a diagnosis can be obtained in most cases. As these symptoms are not specific or exclusive to leukaemia, it is very common for the patient to have visited a doctor several times before being diagnosed. Generally, this does not influence the child’s curative options.
How is B-acute lymphoblastic leukaemia diagnosed?
Generally, if a child presents the characteristic symptoms (anaemia, bleeding, fever, etc.), leukaemia can be diagnosed with a blood test. When the blood is examined under a microscope, leukaemic cells will be visible. Sometimes, at the beginning of the disease, these cells are not seen in the blood and leukaemia is suspected due to the symptoms and some alterations in the blood tests. The diagnosis is confirmed by a bone marrow puncture (iliac crests) and analysis of the cells obtained.
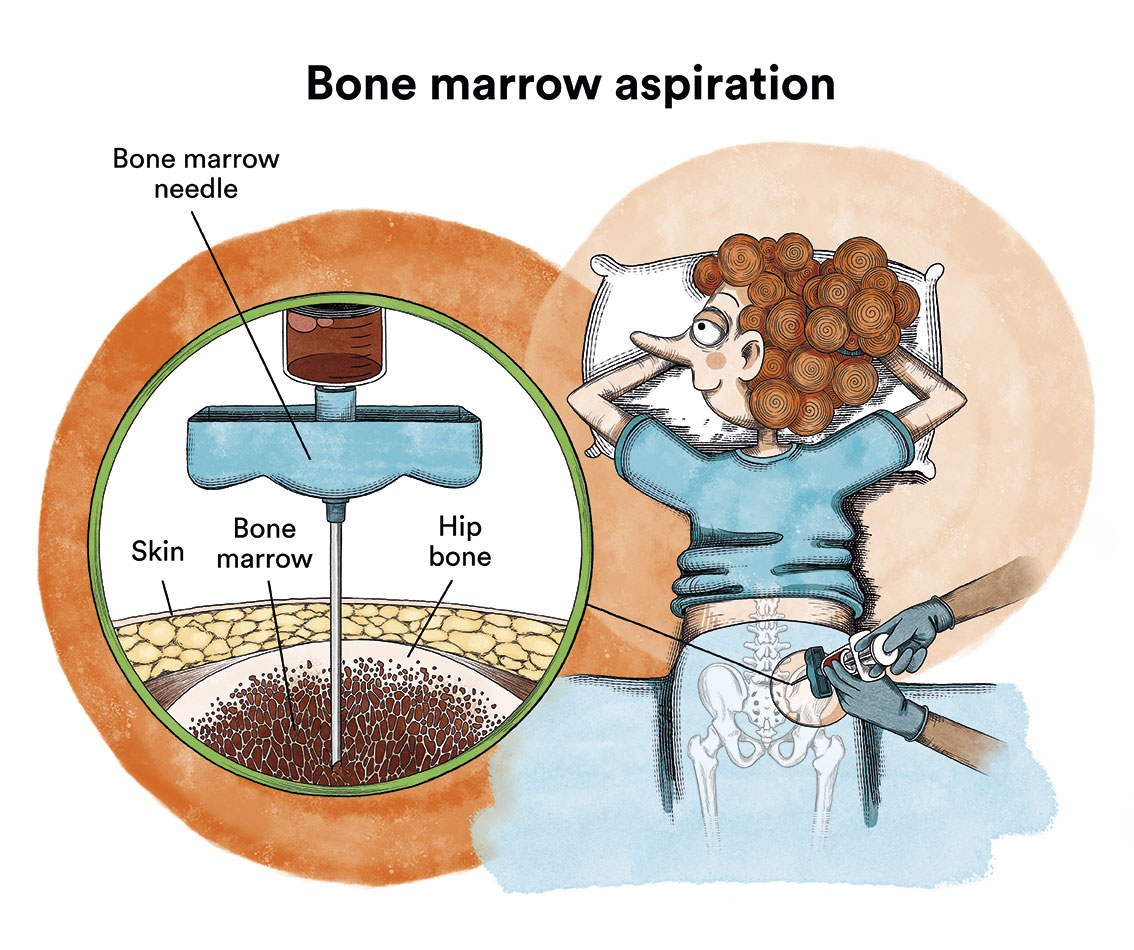
What is the treatment for B-acute lymphoblastic leukaemia in children?
The goal of treatment for acute lymphoblastic leukaemia is to eliminate the leukaemic cells to allow the bone marrow to return to its normal functioning.
The child’s team of haematology doctors will decide on the best treatment for them, taking into consideration many factors, including:
-
- The type of ALL the child has (B or T)
- The child’s age and the number of leukocytes at diagnosis
- The genetic characteristics of the leukaemic cells
- The child’s response to treatment
The treatment of ALL follows treatment protocols developed by paediatric haematology and oncology specialists and is based on the results of other protocols (from national and international groups).
Basically, chemotherapy is the main treatment the child will receive. It involves the use of drugs that kill cancer cells by preventing them from reproducing.

When chemotherapy is administered intravenously, to avoid repeatedly puncturing a vein, specialists implant a special device called a catheter (content in spanish). The catheter is inserted into a large vein, which allows for the administration of all types of medication, as well as for drawing blood for blood tests, thus avoiding the child from enduring repeated needle punctures.
There is a type of catheter, called a port-a-cath, which is attached to a round plastic or metal reservoir under the skin of the chest. The port-a-cath is very practical for children because it is under the skin and does not allow the child to pull it out, it is less likely to become infected than other types of catheters and it allows the child to bathe.
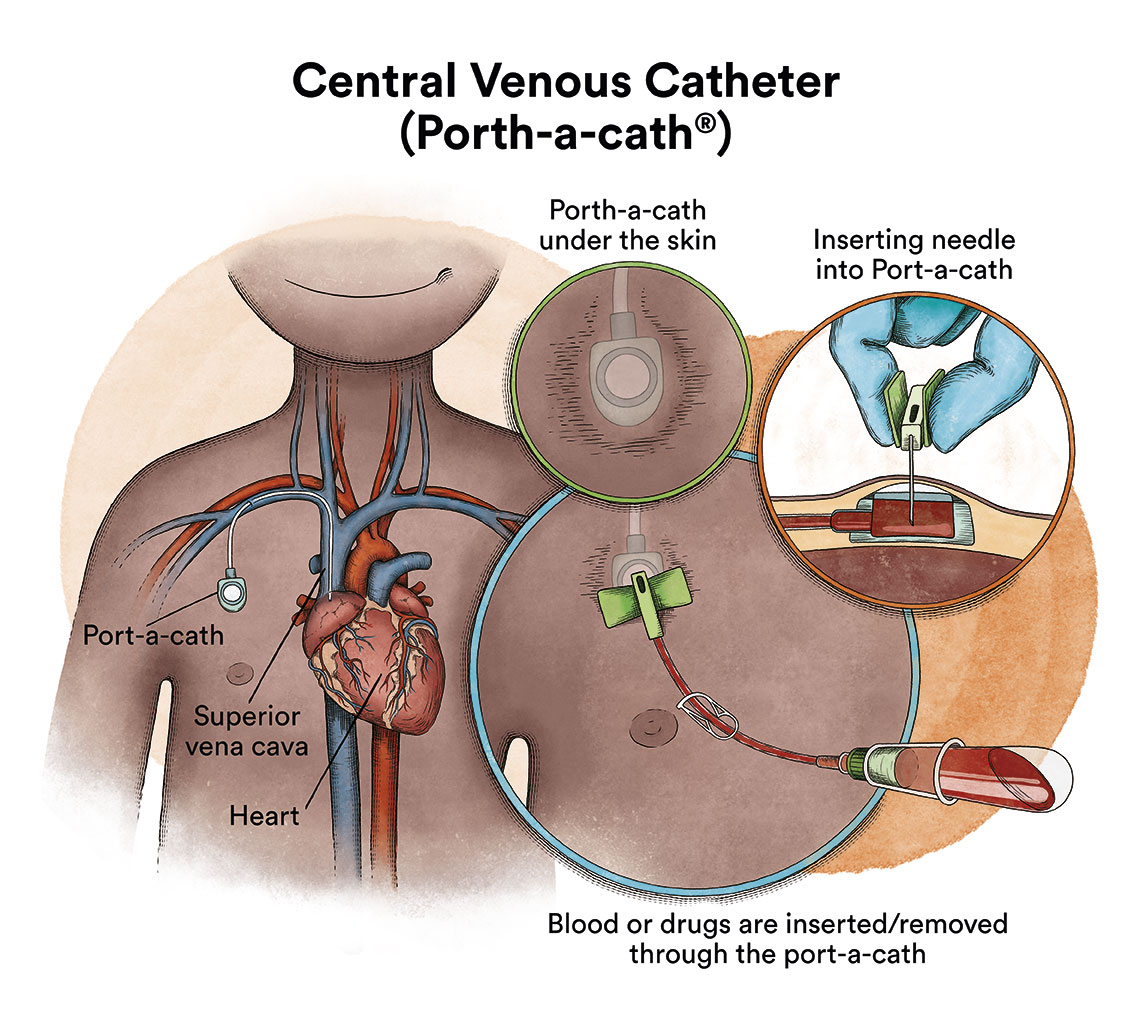
If the chemotherapy is administered through a venous catheter, it reaches almost all the cells of the body via the blood. However, most chemotherapy drugs do not fully reach the cerebrospinal fluid that bathes the brain and spinal cord. This means that there are leukaemic cells that can survive in this fluid. In order to prevent leukaemic cells that reach the cerebrospinal fluid from surviving and causing a future relapse that will affect the nervous system, chemotherapy must be administered directly into the cerebrospinal fluid, via lumbar punctures (intrathecal chemotherapy). In a minority of children who, due to the characteristics of their ALL, are known to have a higher risk of relapse in the nervous system, this treatment can be complemented with cranial radiotherapy.
Chemotherapy treatment can cure up to 85-90% of children with B-ALL. When no leukaemia cells are seen in the bone marrow or elsewhere, the patient is said to be in complete remission.
15-20% of children can relapse from leukaemia. Most relapses occur in the first 5 years after diagnosis, especially in the first 2 years after the end of treatment. In cases of relapse, chemotherapy is re-administered and, depending on the case, a bone marrow transplant is performed (see RELAPSE). There are also new treatment modalities for relapsing children (see NEW TREATMENTS)
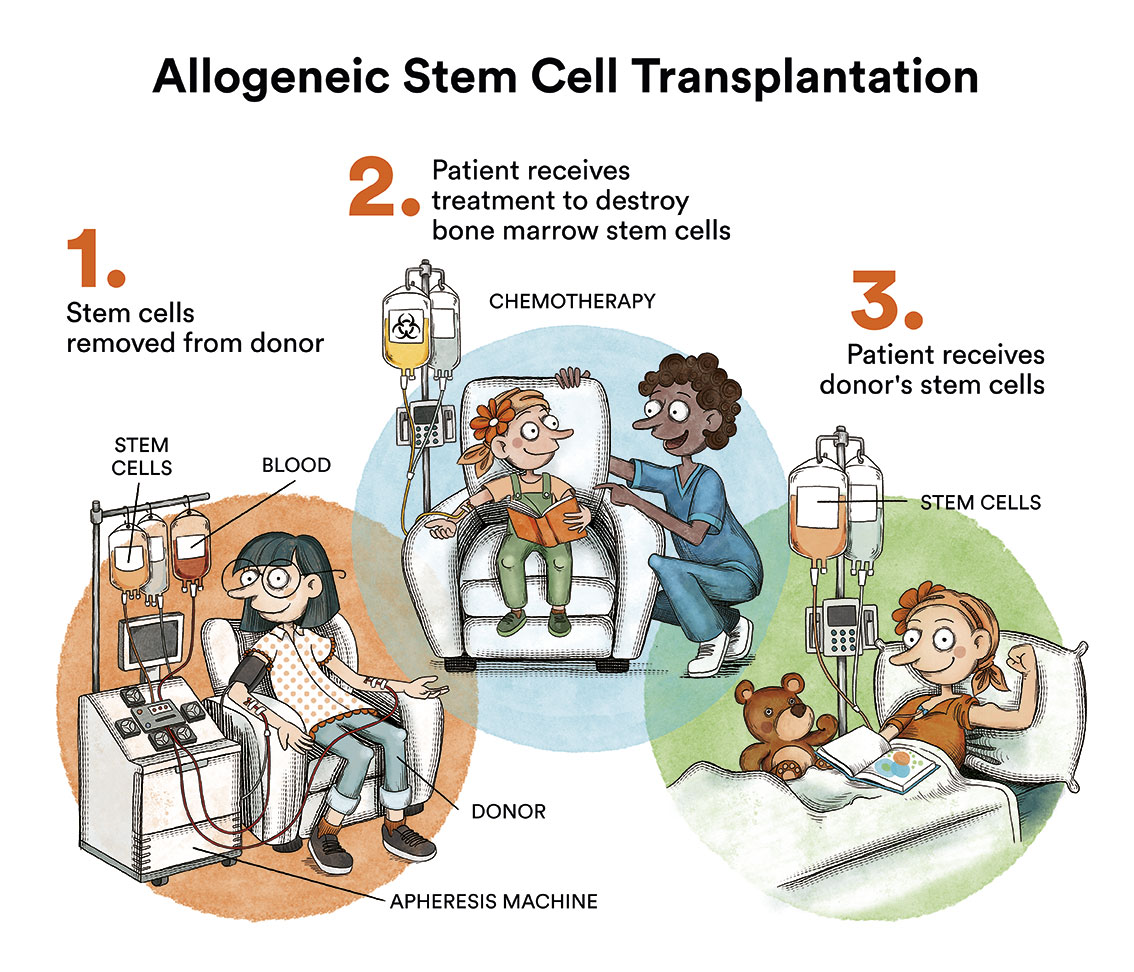
 Most children with ALL have a good chance of being cured with chemotherapy alone and transplantation is not indicated. Transplantation is reserved for cases that are more difficult to cure with chemotherapy alone as it is a more intensive treatment with more risks and possible sequelae.
Most children with ALL have a good chance of being cured with chemotherapy alone and transplantation is not indicated. Transplantation is reserved for cases that are more difficult to cure with chemotherapy alone as it is a more intensive treatment with more risks and possible sequelae.
In children who have relapsed or in those who, due to the characteristics of their leukaemia, we know have a very high risk of relapse, a bone marrow transplant is usually indicated. This is performed once a new complete remission has been achieved with intensive chemotherapy or other treatment modalities. With transplantation, the chances of cure may increase.
Types of chemotherapy
The chemotherapy the patient will receive will depend on the type of leukaemia and the likelihood of relapse. There are different types of treatment, which will be more or less intense, depending on the risk of relapse. Depending on this risk, patients are classified into the following groups:
1) Standard risk
2) Intermediate risk
3) High risk
The intensity and duration of chemotherapy may vary according to the risk group. In any case, all children, irrespective of the risk group into which the are classified, shall be provided with:
1) an initial treatment called induction treatment, of intensive chemotherapy followed by
2) a consolidation or or intensification treatment. This is then followed by:
3) a maintenance treatment which consists of a low intensity chemotherapy, consisting of pills (oral administration), which, in most cases, allows for the child to live an almost normal life, returning to school, sports or other extracurricular activities. In a small group of children with an increased risk of relapse, a bone marrow transplantation is performed instead of the maintenance treatment.
Adrián
Acute Lymphoblastic Leukaemia.
“Adrián was diagnosed with acute leukemia when he was 2 years old. After treatment, he recovered perfectly. He left all medication behind and only went to the hematologist once a month for a check-up. He was already beginning to lead a normal life, in September he had returned to school and the fear had disappeared. But he relapsed. And he had to fight again. The only way was a bone marrow transplant. The Josep Carreras Foundation, in coordination with the National Transplant Organization in Spain, searched around the world for a bone marrow donor compatible with him. The recovery was very difficult because, in addition to several complications, the COVID19 pandemic came together. But now he is home, he has gone back to school, to play sports and he is great.”
What are the chances of B-acute lymphoblastic leukaemia child patients being cured?
Up to 85-90% of children with ALL can be cured. The chances of cure may vary according to age (best prognosis between 1 and 9 years), the number of leukocytes at diagnosis (best if low) and the biological characteristics of the leukaemia (depending on the type of leukaemia and the genetic alterations in the cancer cells). Children under 1 year of age have a somewhat lower chance of cure, as do some children with certain genetic alterations, such as those with the Philadelphia + chromosome. However, with new treatments, most children in these subgroups are also cured. The most important factor influencing prognosis is the treatment given to the child and the child’s response to this treatment. To assess this response, a series of bone marrow punctures will be performed throughout the course of treatment.

What happens if the child relapses?
If the child suffers a relapse of acute lymphoblastic leukaemia, the chances of cure and treatment will depend on several factors, mainly:
- of the time between diagnosis and relapse, the longer the better
- whether it is acute lymphoblastic leukaemia type B or type T
- the location of the relapse (bone marrow or other sites such as the nervous system, testicles or other)
- the child’s response to treatment of the relapse
Treatment will usually consist of more intensive chemotherapy than that initially received and often, bone marrow transplantation. Some relapsed children can be cured without transplantation.
In recent years, in addition to chemotherapy, there are new treatments that can replace or complement chemotherapy, such as immunotherapy and treatments directed against a molecular target (see NEW TREATMENTS).
New treatments for B-acute lymphoblastic leukaemia
In recent years there has been a revolution in the treatment of cancer and specifically B-acute lymphoblastic leukaemia. Among the new treatments available to treat ALL are the treatments known as precision medicine and immunotherapy, especially CAR-T immunotherapy (content in spanish).
Precision medicine is about delivering a personalised treatmenttargeted against genetic alterations present in the patient’s specific cancer or leukaemia. For example, imatinib has significantly increased the cure rate of children with Philadelphia chromosome ALL (Ph+ ALL).
Immunotherapy treatments are cancer treatments that help the immune system fight cancer. The patient’s own immune system is boosted to help their body fight infections and other diseases. Immunotherapy can be used alone or in combination with chemotherapy or other cancer treatments.
There are various therapies such as:
- Monoclonal antibodies and checkpoint inhibitors
When the immune system detects something harmful, it produces antibodies. Antibodies are proteins that fight infection by binding to antigens. These antigens are molecules that initiate the immune response in the body. Monoclonal antibodies are produced in a laboratory to enhance the body’s natural antibodies or act as antibodies in their own right. Some antibodies block the activity of the cancer cells’ proteins, preventing them from reproducing. Others inhibit or stop immune checkpoints. The body uses the immune check-points (check-points) to naturally prevent the immune system from attacking healthy cells. Immune checkpoint inhibitors prevent cancer cells from blocking the immune system. Some of these monoclonal antibodies used in the treatment of acute lymphoblastic leukaemias are rituximab, blinatumomab inotuzumab, among others).
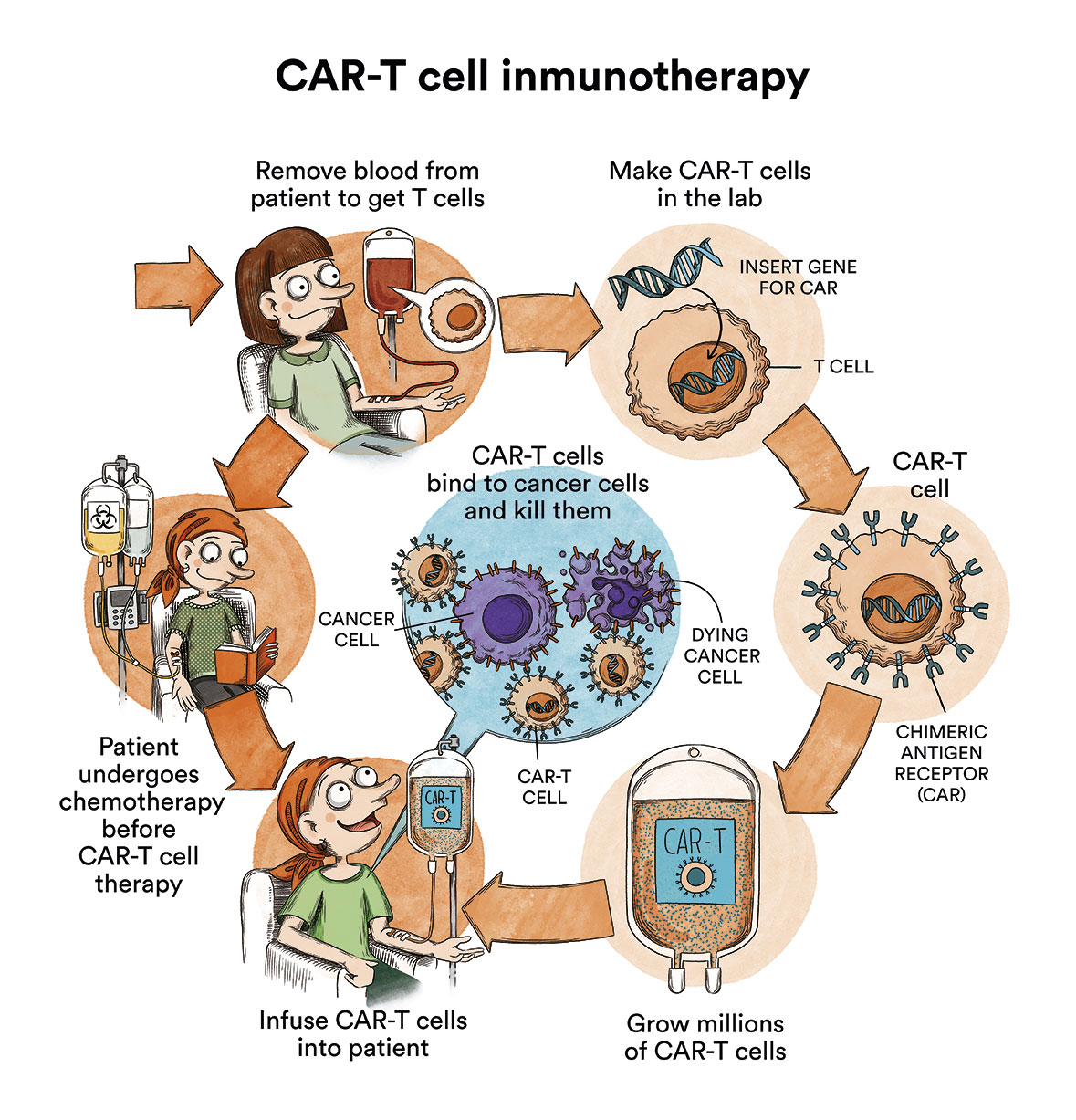
- Cellular therapies such as CAR-T immunotherapy
Among other cell therapies, treatment with CAR-T cells has shown promising results in children with B-type ALL. CAR-T lymphocytes are lymphocytes that are extracted from the patient and genetically modified to recognise and destroy the leukaemic cell. See CAR-T Immunotherapy or how to re-engineer one’s own cells to target cancer (content in spanish)

Abril
Acute myeloid leukemia.
“When I was five months old, I was diagnosed with acute lymphoblastic leukaemia. After undergoing a very hard treatment, I received a blood stem cell transplant from an anonymous donor finded by the REDMO program of the Josep Carreras Foundation. After 4 years of recovery, and when I was already well, the leukemia returned. At that time, I was lucky enough to be able to undergo a CART immunotherapy clinical trial, the first to be done in Spain with children. It was 2016. Since then, I have been fine. I went back to school, to dancing, to music, to reading… and since then I have enjoyed life very much. I am unstoppable.”
Monitoring
After completing the treatment, the child will have regular check-ups performed by their haematologist and by other specialists where necessary. Monitoring is carried out to assess possible relapse and to follow-up and treat possible long-term complications. These checks are progressively spaced out until they are carried out once a year. Long-term follow-up is recommended at least annually in order to early detection and treatment of any sequelae arising from treatment or leukaemia, should they appear.
Recommendations and other practicalities
Here are some general recommendations that answer some of the most frequently asked questions by parents of children with leukaemia:
- Will their hair fall out? When? Should we cut it?
With the chemotherapy they will receive to treat the leukaemia, their hair will fall out. This usually happens 2-3 weeks after the start of chemotherapy. If the child has long hair, it is more appropriate to cut it short before it starts to fall out. It is neither necessary, nor psychologically desirable, to cut it during the first days of admission. Nor does this fact need to be explained to the child straight away. However, it is important to address this issue with the child before their hair starts to fall out. Hair regrows 2-4 weeks after starting the maintenance phase of treatment, where chemotherapy is less intense.
- Hygiene
Since the child’s defences against infection are weakened (due to the illness itself and also due to the treatment administered), it is advisable to maintain adequate hygiene of the child’s body, the hospital room and the family home, including the child’s toys.
It is advisable to avoid dusty toys and cardboard boxes. Food should also not be stored outside the refrigerator. Plants are forbidden in the room, as there are fungal spores in the soil.
Tidiness facilitates cleaning by hospital cleaning staff.
- Visits
It is advisable to reduce the number of visitors in the child’s room, as they may carry infections. It is recommended that there are no more than 2 companions in the room and that they wash their hands before entering. If any of the visitors has an infectious process (cold, conjunctivitis…) it is preferable that they do not visit.
In the case of a parent or other caregiver whose attention cannot be dispensed with, they should wear a mask and wash their hands before coming into contact with the child.
- Food
A child receiving intensive chemotherapy treatment should be provided with a varied diet. When the white blood cell count is low, it is advisable to avoid raw foods that cannot be peeled (e.g. lettuce, strawberries, raw tomatoes).
Sometimes chemotherapy can reduce hunger, or even cause nausea. During the days of chemotherapy, it is not advisable to force your child to eat, as this can be counter-productive.
On the other hand, the corticosteroids (prednisone and dexamethasone) that the child will be administered during some phases of treatment can greatly increase their appetite, even causing anxiety. While they may be allowed to eat more than the meals served in the hospital, they should not be allowed to eat unlimited food, as they will often not tolerate it well and it can cause stomach pain.
Links of interest concerning medical issues relating to acute lymphoblastic leukaemia in children
Childhood Acute Lymphoblastic Leukemia Treatment. National Cancer Institute
Childhood acute lymphoblastic leukaemia (ALL). Cancer Research UK
Childhood acute lymphoblastic leukaemia (ALL). Blood Cancer UK
Acute Lymphoblastic Leukemia (ALL). St Jude Children’s Research Hospital
Links of interest on other topics related to acute lymphoblastic leukaemia in children
CHILDHOOD LEUKAEMIA MATERIAL
- Babies also have leukaemia. Josep Carreras Leukaemia Foundation. (content in Spanish)
- Childhood leukaemia. The little unstoppable ones. Josep Carreras Leukaemia Foundation. (content in Spanish)
- Medulin cut-out set. Josep Carreras Leukaemia Foundation. (content in Spanish)
The Josep Carreras Foundation has a story “The tough baby” aimed at children or siblings suffering from leukaemia. It is especially aimed at children up to the age of 6. If you want to order it, please send us an e-mail to imparables@fcarreras.es.
BONE MARROW TRANSPLANT
- Bone Marrow Transplant Guide. Josep Carreras Leukaemia Foundation.
- What is HLA and how does it work? Josep Carreras Leukaemia Foundation. (content in Spanish)
- Graft-versus-Host Disease Josep Carreras Leukaemia Foundation. (content in Spanish)
- History of Bone Marrow Transplantation. Josep Carreras Leukaemia Foundation. (content in Spanish)
- How is the search for an anonymous donor conducted? Josep Carreras Leukaemia Foundation. (content in Spanish)
- Care guide for transplanted children. TransplantCHild.
- Stem cell transplantation: a colouring book. Leukaemia and Lymphoma Society.
SUPPORT MANUALS
- How to deal with leukaemia and lymphoma in children? Leukemia & Lymphoma Society.
- LIVING BY LEARNING. Action protocol for students with cancer AFANION.
- Support guide for parents of children with cancer ASION.
- A guide for young people and adolescents with cancer ASION.
- Pupils with cancer. A guide for teachers ASION.
- The importance of parental behaviour when a child has cancer ASION.
- My child has cancer. What do I do? FARO.
FOOD
- How to maintain a healthy diet during treatment? Josep Carreras Leukaemia Foundation. (content in Spanish)
- “Bon appetit”. Dietary advice during treatment AFANION.
- ‘Jabel’s magic recipes’. Isabel Rojas Murcia, Carolina Mangas Gallardo.
OTHER
- Information on the long-term and late effects of treatment for leukaemia/lymphoma in children Leukemia & Lymphoma Society.
- My sibling has cancer Josep Carreras Leukaemia Foundation. (content in Spanish)
- School in a hospital Josep Carreras Leukaemia Foundation. (content in Spanish)
- Educating illusions. Guide for psycho-educational intervention in children and adolescents with cancer FARO.
- Cancer in adolescents Josep Carreras Leukaemia Foundation. (content in Spanish)
- ‘Leukaemia and adolescents’ documentary Josep Carreras Leukaemia Foundation.
- ‘Babies also have leukaemia’ documentary Josep Carreras Leukaemia Foundation.
- 7 ways to wear a scarf Josep Carreras Leukaemia Foundation. (content in Spanish)
- ‘Princess Luzie and the chemo knights’ story ASPANAFOA.
- ‘Let’s go to chemotherapy’ story.
- ‘Let’s go to radiotherapy’ story.
- ‘Gasparín Super Quimio’ story Spanish Federation of Parents of Children with Cancer.
- ‘Charlie Brown and leukaemia’ story.
- ‘Toby and the flying machine’ story.
- ‘The fairy of the stars’ story AECC.
- ‘Lina the little swallow’ story Osakidetza.
Useful links: local entities (resources and services)
All these organisations are external to the Josep Carreras Leukaemia Foundation.
ANDALUCÍA
ARAGÓN
ASTURIAS
CASTILLA LA MANCHA
CASTILLA LEÓN
CATALUÑA
VALENCIAN COMMUNITY
EXTREMADURA
GALICIA
BALEARIC ISLANDS
CANARY ISLANDS
LA RIOJA
MADRID
- AAA (asociación de adolescentes y Adultos Jóvenes con Cáncer)
- ASION
- FUNDACIÓN CAICO
- FUNDACIÓN ALADINA
- FUNDACIÓN UNOENTRECIENMIL
MURCIA
NAVARRA
BASQUE COUNTRY
Support and assistance
We also invite you to follow us through our main social media (Facebook, Twitter and Instagram) where we often share testimonies of overcoming this disease.
If you live in Spain, you can also contact us by sending an e-mail to imparables@fcarreras.es so that we can help you get in touch with other people who have overcome this disease.
* In accordance with Law 34/2002 on Information Society Services and Electronic Commerce (LSSICE), the Josep Carreras Leukemia Foundation informs that all medical information available on www.fcarreras.org has been reviewed and accredited by Dr. Enric Carreras Pons, Member No. 9438, Barcelona, Doctor in Medicine and Surgery, Specialist in Internal Medicine, Specialist in Hematology and Hemotherapy and Senior Consultant of the Foundation; and by Dr. Rocío Parody Porras, Member No. 35205, Barcelona, Doctor in Medicine and Surgery, Specialist in Hematology and Hemotherapy and attached to the Medical Directorate of the Registry of Bone Marrow Donors (REDMO) of the Foundation).
Become a member of the cure for leukaemia!


