Haematopoietic progenitor-cell transplantation
Haematopoietic progenitor-cell transplantation, traditionally known as bone marrow transplantation, is a therapy that is mainly used for treating blood cancers such as leukaemias or lymphomas.
The information provided on www.fcarreras.org is intended to support, not replace, the relationship that exists between patients/visitors to this website and their physician.

Adrián
Acute lymphoblastic leukemia.
“Hi, my name is Adrian. I never thought that, at Christmas 2018, I would change the Philippines for a hospital room. Temporarily back in my city to enjoy my loved ones, on December 28 I was diagnosed with acute lymphoblastic leukemia. Can you imagine the shock? For 8 months, sand, coconuts and sea became needles, chemotherapy, pills and finally a bone marrow transplant. I could not be more grateful to my anonymous donor for giving me this new opportunity to live, to my family, to the great professionals at the hospital and to the Josep Carreras Foundation for their great work in research and support for hematological diseases. Now, a few years have passed since the transplant, I feel great, and I have resumed my life completely, working in the world of film production”.
Information reviewed by Dr. Rocío Parody Porras, Doctor specialising in Haematology. Member of the Management of REDMO (Bone Marrow Donor Registry) and of the Foundation’s medical team. Barcelona Medical Association (Co. 35205)
What is a haematopoietic progenitor-cell transplant and what is its purpose?
Haematopoietic transplantation (bone marrow, umbilical cord blood or peripheral blood transplantation) is a treatment option that can be applied in certain patients with a blood cancer process. The patient’s bone marrow, which produces malignant cells, is destroyed by administering high doses of drugs (chemotherapy…) and/or radiotherapy, and replaced by healthy bone marrow. This procedure consists of: replacing the body’s blood cell factory.
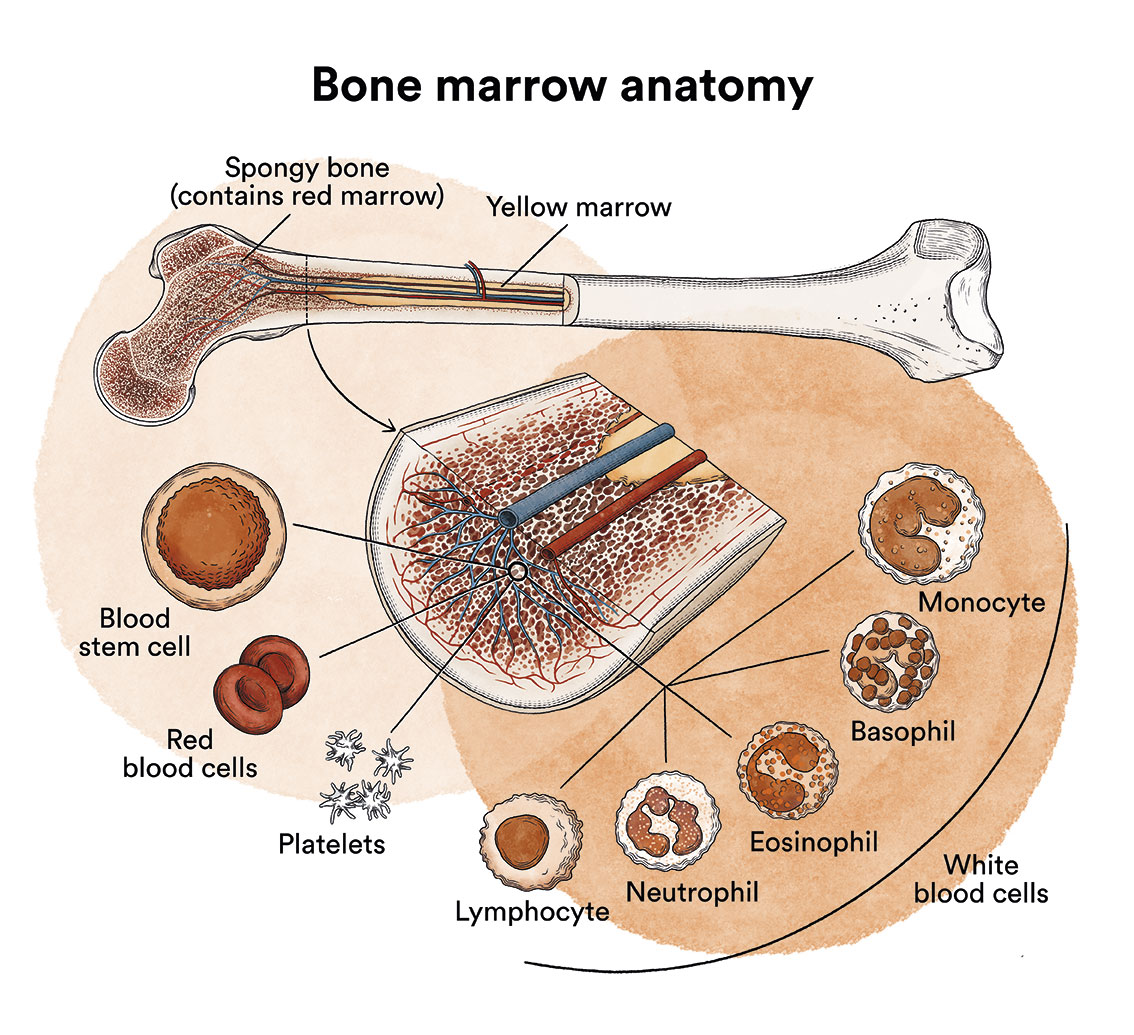
Healthy bone marrow can come from a donor (allogeneic transplantation) or from the actual patient (autogenic or autologous transplantation). In Leukaemia, bone marrow and blood cells you can find out what it is and how bone marrow works. As you will see, in no case should it be confused with the spinal cord.
While haematopoietic transplants were traditionally performed using haematopoietic progenitor cells from bone marrow (bone marrow transplantation), nowadays transplants are mainly performed with progenitors obtained from venous blood, after stimulating the passage of haematopoietic progenitors from the bone marrow into the blood (peripheral blood), or in rarer situations, from umbilical cord blood, which is very rich in haematopoietic progenitors, obtained at the time of birth.
We recommend that you carefully read the online “Bone marrow transplant guide for the patient” (content in Spanish) by the Josep Carreras Foundation.
What types of haematopoietic progenitor-cell transplantations are there?
Primarily we have to differentiate between autologous transplantation (from the patient’s own cells) and allogeneic transplantation (from a donor). The latter can, in turn, be from a family donor, mainly a sibling, or from an anonymous histocompatible donor. Recently, in some specific cases, allogeneic haploidentical transplants have also started to be performed in which the donor is only 50% compatible.
- Autologous transplantation or autotransplantation:
“Auto” means “oneself”. Stem cells are taken from oneself before receiving high-dose radiotherapy or chemotherapy treatment and are stored (cryopreservation). After performing the high-dose radiotherapy or chemotherapy, the stem cells are put back into the body to be added to the normal blood cells. This is called “rescue” transplant. In an autologous transplant, patients receive their own stem cells. An autologous transplant aims to eliminate neoplastic cells by means of high doses of chemotherapy, with or without radiotherapy, and to recover bone marrow function as soon as possible, thanks to the patient’s own blood stem cells. In some diseases, the dose of chemo-radiotherapy necessary for cure is so high that it would cause the death of the patient due to its toxicity on the bone marrow. It should be noted that chemo-radiotherapy, in addition to the abnormal cells, also destroys (albeit to a lesser extent) the body’s normal cells, especially those of the bone marrow (myeloablation), producing an extreme pancytopaenia (lack of red blood cells, leukocytes and platelets), which is incompatible with life. The simplest way to resolve this irreversible bone marrow toxicity is to administer, after intensive treatment (or conditioning treatment), stem cells from the patient’s own blood for achieving “haematopoietic rescue”. While this procedure cures some diseases, such as various types of lymphomas, it does not cure most leukaemias or non-neoplastic congenital haemopathies.
Autologous transplantation is also commonly used in multiple myeloma patients and, although it does not have curative properties, it serves to prolong disease remission.
An advantage of autologous stem cell transplantation is that the patient is supplied with his or her own cells, so there is no risk of ‘rejection’.
Jesús
Multiple Myeloma.
“I am Jesús, I am 42 years old and I am a Multiple Myeloma patient. I was diagnosed when I was 32 years old and it was a great shock for me. I was terrified of doctors, and I had never had my blood drawn. My life changed radically overnight. Thanks to my hematologist, I was aware that the diagnosis was serious, but there were treatments and chances to live. After a few previous cycles of chemo I underwent an autologous bone marrow transplant and was in complete remission for 9 years.
I recovered perfectly and my quality of life remained the same. I now lead a completely normal life and simply go for regular check-ups to make sure everything is OK. I underwent a second autologous bone marrow transplant 9 months ago because I had a small relapse, and everything went well again. It is clear to me that I was able to have this treatment thanks to the research that someone was able to carry out at the time, thanks to the efforts of many associations that do their bit by financing many trials and tests, informing, and encouraging many people to become bone marrow donors, such as the Josep Carreras Foundation”.
- Allogeneic histocompatible donor transplantation or allogeneic transplantation:
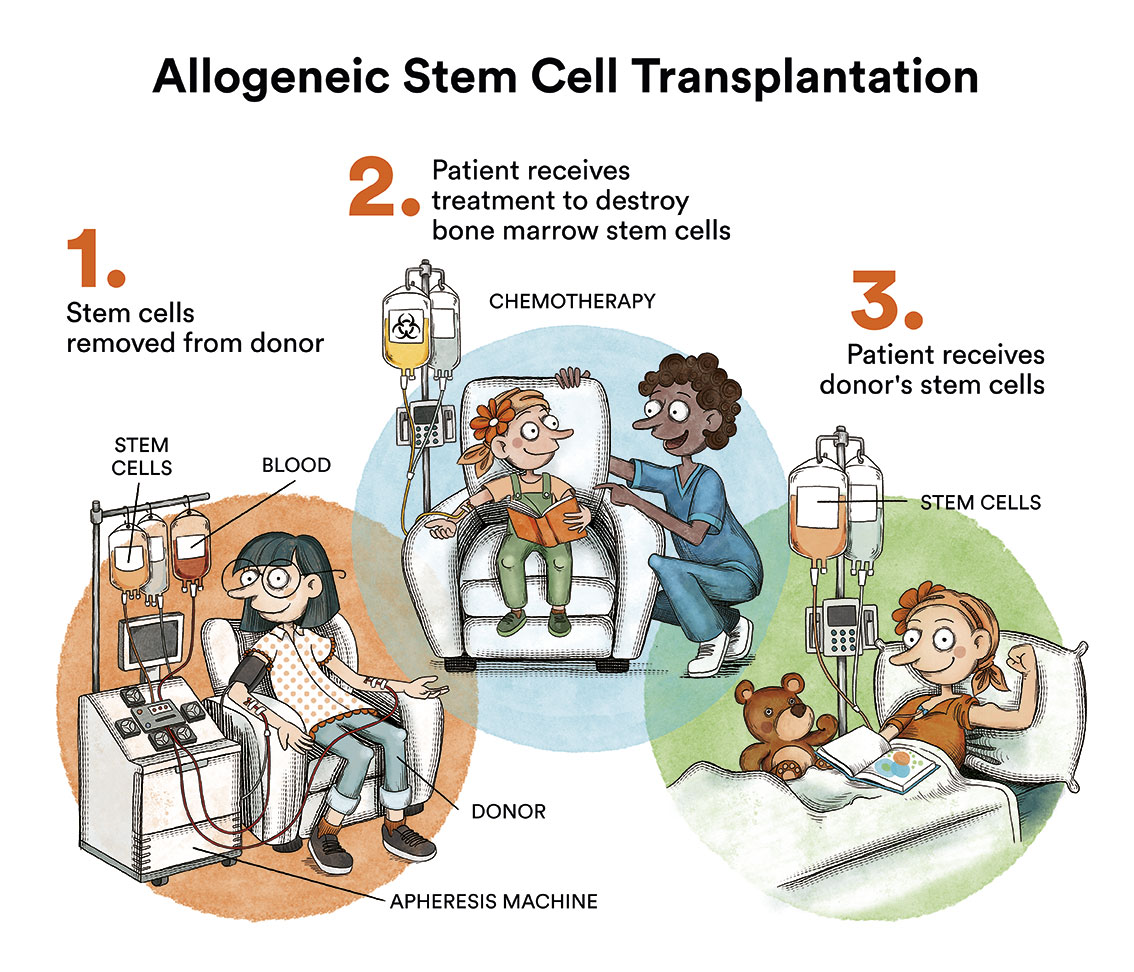
An allogeneic transplant (or allotransplantation of stem cells (by extraction of bone marrow, peripheral blood or umbilical cord blood) is a transplant from a donor. “Alo” means “other”, “different”. This procedure aims to partially or totally eliminate diseased cells thanks to chemotherapy and/or radiotherapy and replace them with other normal cells sourced from a healthy donor. To ensure that the transplant works well and that the body does not “reject” the new marrow (known as Graft-versus-Host Disease (content in spanish) – GVHD), the highest degree of HLA compatibility (content in spanish) (histocompatibility) between patient and donor is usually sought. Usually, if the patient has siblings (from the same father and mother), the first thing the haematology team will do is request the HLA typing of the siblings to check if any of them are 100% compatible. This situation will only occur in 25% of cases. Other patients who do not have a suitable donor among their relatives will have to opt for searching for an anonymous, voluntary donor around the world through international registries. In Spain, the official register is REDMO (Bone Marrow Donor Registry), a programme created in 1994 and managed by the Josep Carreras Foundation, which works in coordination with the ONT (National Transplant Organisation) and the Spanish Autonomous Communities. REDMO works with and conducts searches for all Spanish public hospitals that perform allogeneic bone marrow transplants. All searches are conducted at the same time among all available donors worldwide: more than 40 million. The prospect of finding a histocompatible donor is currently high. In the following video you can see how a donor search is carried out.
On a practical level, an allogeneic transplant works in much the same way as an autologous transplant. Stem cells (from bone marrow or peripheral blood) are collected from the donor and stored or frozen. After receiving high doses of chemotherapy and/or radiotherapy, which is known as transplant conditioning, the donor stem cells will be thawed so that they can be delivered to the patient usually through a catheter (content in spanish).
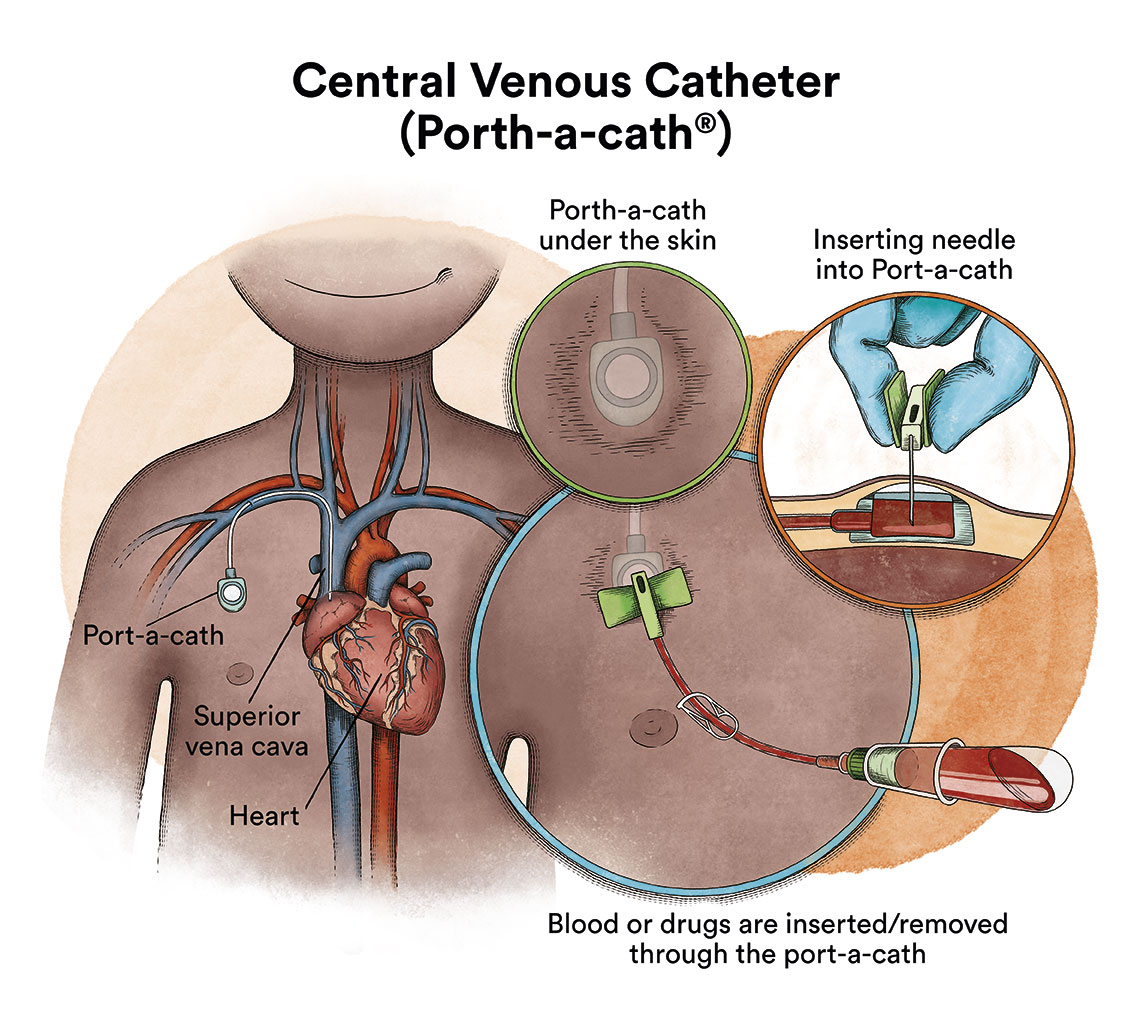
Allogeneic stem cell transplantation is often the only chance for curing many diseases, especially acute leukaemias and high-risk myelodysplastic syndromes, some types of lymphoma and others.

Álvaro, 52 years old
Acute Myeloid Leukaemia.
“During the entire healing process of my leukemia, from a bone marrow transplant from an anonymous donor, I only had one totem: Here and now. I invite you to share my experience reading my Ebook (in Spanish)”
- Allogeneic transplantation from a haploidentical donor:
“Haplo” means “half”. A transplant from a haploidentical donor is a transplant from a donor that is half histocompatibility (content in spanish) identical. This happens with parents (as you inherit half from each), with offspring and potentially with siblings (with whom you can be identical, share only half, i.e. haploidentical, or not share any part at all). The activity of this type of transplantation has increased in the last decade thanks to new and more powerful anti-rejection treatment strategies, with this being a donor alternative in the absence of a 100% compatible donor or due to the urgency of the case, for example a disease with a high risk of immediate progression and that cannot wait for the search for a donor. This therapeutic alternative is very interesting for example in patients with an under-represented ethnicity in the world bone marrow registries for whom it is sometimes not easy to find a 100% compatible donor.
To overcome this lack of compatibility, a specific “anti-rejection” strategy is essential. Traditionally, the product was either manipulated to eliminate the T-lymphocytes responsible for rejection, or intensive immunosuppressive treatment was used to minimise the presence of these cells in the product infused into the patient due to the high risk of developing Graft-Versus-Host Disease (content in spanish). However, nowadays, with the use of a cytostatic drug called cyclophosphamide, which is administered a few specific days after transplantation (third and fourth day), it is possible to eliminate these T lymphocytes (called allo-reactive) and this, followed by daily immunosuppressive treatment maintained over time, has radically changed the outcome of this type of transplant with overall results that are close to the results of transplants from an identical donor.
Anna
Acute myeloid leukemia.
“When I was 27 years old, in 2015, my life and the lives of mine changed radically: I was diagnosed with acute myeloid leukemia. After several chemotherapy sessions, we were told that a bone marrow transplant had to be done, which we already knew I would need sooner or later, but we couldn’t wait long. The Josep Carreras Foundation, through the REDMO program, was looking for a 100% compatible donor in the world donor bank, but no luck. Therefore, the other option was the haploidentical donor. They did the HLA tests on my two sisters and my parents. The coincidence was that my two sisters were 100% compatible with each other, but not with me. After studying the case, they decided that the best donor for me was Maria, my younger sister. I was born again thanks to her”.
For which diseases may autologous progenitor transplantation be needed?
 It is indicated for all those diseases that require such intensive chemo-radiotherapy for their cure that it causes irreversible marrow toxicity, but which do not require the anti-tumour action of healthy donor cells. This is the case for many lymphomas, some acute leukaemias and some solid tumours. In many cases, autologous transplantation is used for the sole purpose of temporarily controlling the disease because other options are not considered valid or are unacceptable due to the risks involved. This is the case for diseases such as multiple myeloma, amyloidosis or certain autoimmune diseases, among others.
It is indicated for all those diseases that require such intensive chemo-radiotherapy for their cure that it causes irreversible marrow toxicity, but which do not require the anti-tumour action of healthy donor cells. This is the case for many lymphomas, some acute leukaemias and some solid tumours. In many cases, autologous transplantation is used for the sole purpose of temporarily controlling the disease because other options are not considered valid or are unacceptable due to the risks involved. This is the case for diseases such as multiple myeloma, amyloidosis or certain autoimmune diseases, among others.
For which diseases may allogeneic bone marrow transplantation be needed?
Donor bone marrow transplantation is one of the treatments of choice for various types of leukaemia, but this is not the only disease that can be cured by this procedure.
- Leukaemias
Acute leukaemias (acute lymphoblastic leukaemia – ALL or acute myeloid leukaemia – AML) account for the majority of cases for which allogeneic stem cell transplantation is indicated. In fact, more than 50% of the searches for an anonymous compatible donor carried out by the Bone Marrow Donor Registry (REDMO) each year are for patients with acute leukaemia.
The leukaemias that may be susceptible to the patient having to undergo haematopoietic stem cell transplantation are essentially: acute myeloid leukaemia and acute lymphoblastic leukaemia – ALL when it is high risk.
Not all patients with leukaemia require an allogeneic (donor) haematopoietic stem cell transplant. For example, only 10% of children with acute lymphoblastic leukaemia (ALL) require this procedure. In addition, patients with certain acute leukaemias, such as acute promyelocytic leukaemia, do not currently require an allogeneic transplant. This is also the case for most chronic leukaemias such as chronic myeloid leukaemia and chronic lymphocytic leukaemia. Taking this into account and the fact that patients over 70 years of age cannot, in principle, undergo such a transplant, we can say that 20% of patients with acute leukaemia require an allogeneic transplant.
- Lymphomas
Lymphomas are a group of neoplastic diseases (cancers) that develop in the lymphatic system, which is part of the human body’s immune system. There are two main types of lymphoma: Hodgkin’s lymphoma (HL) and non-Hodgkin’s lymphoma (NHL). Normally, patients with Hodgkin’s lymphoma do not usually undergo an allogeneic transplant as the disease can be cured with chemotherapy and/or autologous progenitor transplantation, although in cases where these treatments have not worked, a family or unrelated donor transplant can be given. Moreover, nowadays, with the advances in immunotherapy, particularly CART therapy (content in spanish), the indication for transplantation, especially allogeneic transplantation, is becoming very rare in this disease.
Lymphoma patients undergoing allogeneic transplantation each year account for about 10% of transplant indications, while they are the second most frequent indication for autologous haematopoietic stem cell transplantation.
In the case of diffuse large B-cell lymphoma (the most common histological type of lymphoma), the standard indication accepted by most transplant organisations and scientific societies includes autologous transplantation in patients after a first relapse, which occurs in almost 50% of patients with this subtype of lymphoma, although this indication may change in the near future with the incorporation of CART (content in spanish). In all other histological subtypes, the indication depends on a multitude of factors, hence the decision to transplant must, in many cases, be individualised and considered based on each patient’s context.
- Myelodysplastic syndromes
In myelodysplastic syndromes (MDS), the blood stem cells produced by the bone marrow and responsible for making all blood cells do not mature and therefore do not develop into healthy red blood cells, white blood cells or platelets.
In general, mild cases of MDS usually do not require any treatment and may remain stable for years. The only curative treatment for MDS is allogeneic haematopoietic stem cell transplantation, but the advanced age of many patients and the toxicity of this procedure limit its use to young patients with poor prognosis MDS who have a suitable donor, with these constituting slightly less than a quarter of patients.
- Bone marrow aplasia
Bone marrow aplasia (or MA) is the disappearance of the bone marrow stem cells responsible for the production of all blood cells. Patients with non-severe aplasia may be virtually asymptomatic and require no supportive measures. The treatment of choice for severe and very severe bone marrow aplasia in young patients is bone marrow transplantation. In this case, the preferred source of progenitors continues to be bone marrow.
- Congenital erythrocyte abnormalities
Erythrocytes (also called red blood cells or haematids) are the most numerous elements of blood. Haemoglobin is one of its main components, and its purpose is to transport oxygen to the different tissues of the body. Congenital erythrocyte abnormalities that may result in the patient having to undergo haematopoietic stem cell transplantation, ideally bone marrow transplantation, are Fanconi anaemia, Alpha-thalassaemia, Beta-thalassaemia major, sickle cell disease and sideroblastic anaemias.
- Alterations in plasma cells
Plasma cell disorders or monoclonal gammopathies are a group of diseases that includes various haematological malignancies characterised by a disorder of plasma cells and immunoglobulins.
Malignant monoclonal gammopathies that may require haematopoietic stem cell transplantation include multiple myeloma, currently the first indication for autologous transplantation, plasma cell leukaemia, Waldeström macroglobulinemia and amyloidosis.
- Congenital immunodeficiencies
Immunodeficiency is a state in which the immune system does not fulfil its protective role, leaving the body vulnerable to infection. Primary (or congenital) immunodeficiencies manifest themselves, with some exceptions, from infancy onwards, and are due to congenital defects that prevent the immune system from functioning properly.
There are different types of congenital immunodeficiencies but, for the most part, they are extremely rare. Severe Combined Immunodeficiency (SCID) is the most common disease in this group and allogeneic progenitor transplantation, ideally bone marrow, is inevitable for a cure.
- Other ailments
We could cite many other diseases in which a haematopoietic stem cell transplant is often the only chance of cure for the patient, but many of them are in the minority, these being other neoplasms such as primary myelofibrosis or idiopathic myelofibrosis, histiocytosis, metabolic depository diseases or other non-neoplastic diseases.
Of course, this information cannot in any way replace a consultation with a medical specialist. A patient’s haematologist decides which intervention is appropriate depending on the patient’s age, physical condition and disease progression, in agreement with the transplant referral centre if it is not the same centre where the patient is being treated. The decision for a transplant must be consensual.
What is HLA compatibility and why is it important?
Our body’s immune system is a recognition and response system that differentiates between self and non-self and ensures the body’s defence against foreign agents such as infectious micro-organisms, neoplastic (cancer) cells, or normal cells transplanted from another person.
In allogeneic bone marrow transplants (from a donor), maximum HLA (human leukocyte antigen system) compatibility is required. You can read more about how the HLA system works and why some siblings are or are not compatible in our blog: What is HLA and how does it work? (content in spanish)
What is Graft-versus-Host Disease?
Graft-versus-Host Disease (GVHD) is a relatively common complication (occurring in 30-60% of cases) following blood stem cell transplantation (bone marrow, peripheral blood or umbilical cord blood), and can be very serious, even fatal, although most cases respond to corticosteroid treatment which remains the treatment of choice. Basically, it occurs because the donor’s T-lymphocytes (called allo-reactive) recognise markers on the recipient’s cells as “foreign”.
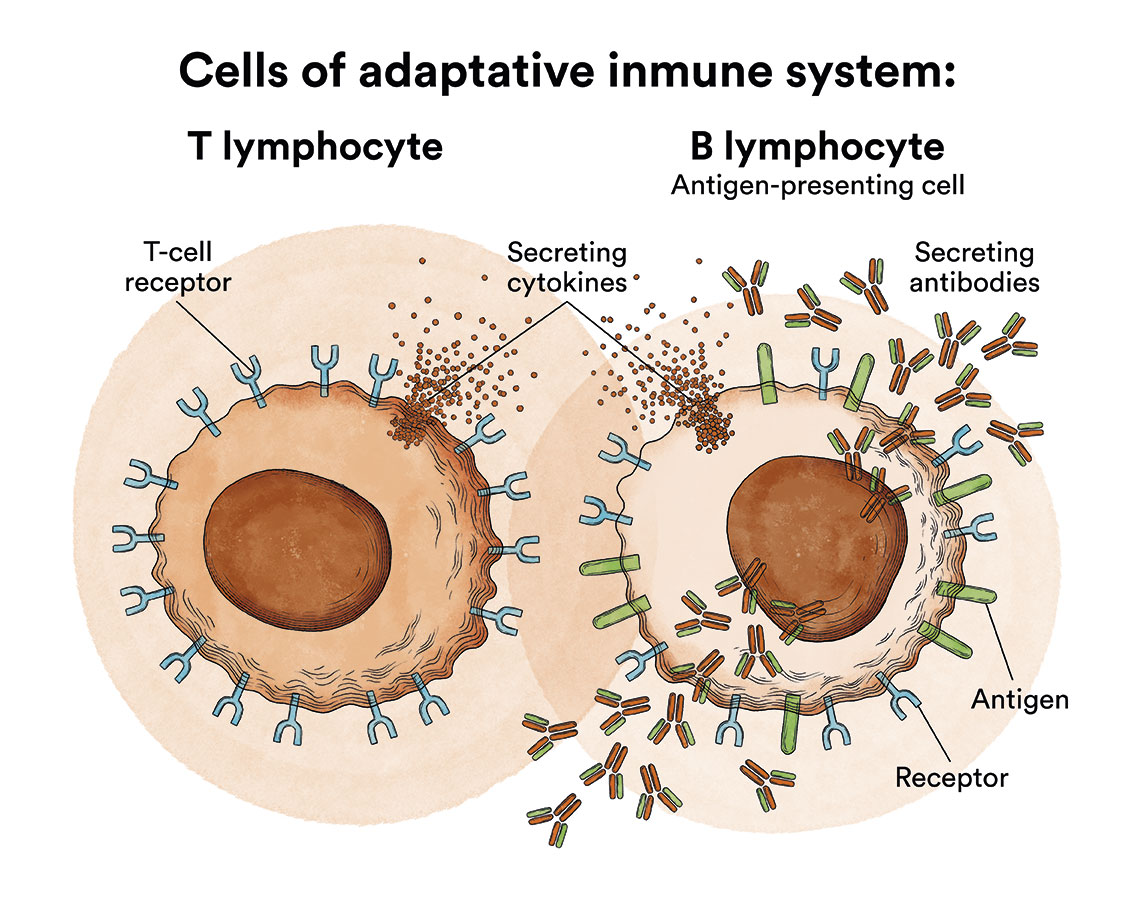
For this reason, after allogeneic transplantation it is necessary to use immunosuppressive (“anti-rejection”) treatment such as cyclosporine, tacrolimus, mycophenolate, which will be maintained for a variable period of time depending on the tolerance and evolution of each patient and their underlying disease. GVHD can be acute (occurring mostly in the first 100 days after transplantation) and chronic, with different manifestations and degrees, and can occur at any time after transplantation, i.e., from the time the new marrow begins to function. It is a frequent reason for consultation once the patient has been discharged, and also for hospital admission when the patient requires intravenous treatment (e.g. gastrointestinal involvement preventing oral tolerance). Acute GVHD manifests itself mainly on the skin (redness and itching, as if you have been in the sun), followed by the gastrointestinal tract (nausea, diarrhoea) and liver (increased bilirubin in the blood, which can lead to yellowing of the skin, known as jaundice). The chronic form has multiple forms of manifestation and can lead to years of immunosuppressive treatment. In the Foundation’s blog you will find a simple and informative explanation to understand the importance of HLA compatibility and why Graft-versus-Host Disease (content in spanish) (GVHD) occurs.
Who searches for an HLA-compatible donor and how?
As explained above, often the only chance of cure for many patients with leukaemia or other haematological malignancies is a bone marrow, peripheral blood or umbilical cord blood (haematopoietic progenitor) transplant. However, 3 out of 4 patients will not have a compatible family member.
Faced with this situation, in 1991, the Josep Carreras Leukaemia Foundation created the Bone Marrow Donor Registry (REDMO) (in Spanish) in Spain.

Its objective? To ensure that all patients with leukaemia (or other blood diseases) who needed an allogeneic transplant for a cure and lacked a compatible family donor could access one through a bone marrow donation from a voluntary unrelated donor. Over the years, peripheral blood and umbilical cord blood units, cryopreserved in umbilical cord banks, were added to bone marrow, further facilitating access to this type of transplantation. Until the creation of REDMO, Spanish patients could not access the donor registries that other developed countries had already created. Obviously, this was a major limitation to the cure of a very large number of patients.
The Josep Carreras Foundation was able to establish collaboration mechanisms with donor registries in various European countries and North America, which allowed it to offer patients and medical teams the possibility of accessing the millions of donors who at that time had already given their consent to donate bone marrow in the event that a patient anywhere in the world needed it.
The full development of the REDMO was achieved in 1994 with its integration into the public healthcare network of the National Health System, through the signing of the first Framework Agreement between the Josep Carreras Foundation and the Ministry of Health, through the National Transplant Organisation (ONT).
This Agreement establishes that REDMO is responsible for managing the database of Spanish voluntary donors, for the search for compatible donors for Spanish patients and for coordinating the transport of bone marrow, peripheral blood or umbilical cord blood from the place of collection to the transplant centre. In addition, the Foundation has signed collaboration agreements with all the Autonomous Communities to guarantee coordination in the search for unrelated donors and the procurement and transport of the product.
The searches carried out by REDMO are mainly financed by the budgets of the public health system, specifically the hospitals that request them.
The Bone Marrow Donor Registry (REDMO) is the only programme authorised in Spain to manage searches for unrelated blood stem cell donors for patients treated in Spanish centres that require it, and the only donor registry authorised to manage blood stem cell collections from donors residing in our country. REDMO is interconnected with the international network of registries and can therefore access voluntary donors and umbilical cord blood units available anywhere in the world: more than 40 million donors and more than 700,000 umbilical cord blood units. REDMO also receives requests from registries in other countries to search for compatible Spanish donors for foreign patients.
In the last 35 years, more than 13,000 transplants have been carried out worldwide thanks to an anonymous donor located by the Josep Carreras Foundation’s Bone Marrow Donor Registry.
- REDMO Annual reports. Josep Carreras Foundation
Useful links on haematopoietic progenitor-cell transplantation
Stem Cell or Bone Marrow Transplant. American Cancer Society
Blood-Forming Stem Cell Transplants. National Cancer Institute
Blood and Marrow Stem Cell Transplantation. Leukemia & Lymphoma Society
Blood stem cell and bone marrow transplants. Blood Cancer UK
Links of interest: local/provincial or state entities that can provide you with resources and services specialised in leukaemia or cancer patients:
In Spain there is a large network of associations for haematological cancer patients that, in many cases, can inform you, advise you and even carry out certain procedures. These are the contacts of some of them by Autonomous Communities:
All these organisations are external to the Josep Carreras Foundation.
STATE
- AMILO (Asociación Española de Amiloidosis)
- AEAL (ASOCIACIÓN ESPAÑOLA DE AFECTADOS POR LINFOMA, MIELOMA y LEUCEMIA)
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact with the nearest branch or call 900 100 036 (24h).
- AELCLES (Agrupación Española contra la Leucemia y Enfermedades de la Sangre)
- CEMMP (Comunidad Española de Pacientes de Mieloma Múltiple)
- Josep Carreras Leukaemia Foundation
- FUNDACIÓN SANDRA IBARRA
- GEPAC (GRUPO ESPAÑOL DE PACIENTES CON CÁNCER)
- MPN España (Asociación de Afectados Por Neoplasias Mieloproliferativas Crónicas)
ANDALUCÍA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ALUSVI (ASOCIACIÓN LUCHA Y SONRÍE POR LA VIDA). Sevilla
- APOLEU (ASOCIACIÓN DE APOYO A PACIENTES Y FAMILIARES DE LEUCEMIA). Cádiz
ARAGÓN
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ASPHER (ASOCIACIÓN DE PACIENTES DE ENFERMEDADES HEMATOLÓGICAS RARAS DE ARAGÓN)
- DONA MÉDULA ARAGÓN
ASTURIAS
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ASTHEHA (ASOCIACIÓN DE TRASPLANTADOS HEMATOPOYÉTICOS Y ENFERMOS HEMATOLÓGICOS DE ASTURIAS)
CANTABRIA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
CASTILLA LA MANCHA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
CASTILLA LEÓN
- ABACES (ASOCIACIÓN BERCIANA DE AYUDA CONTRA LAS ENFERMEDADES DE LA SANGRE)
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ALCLES (ASOCIACIÓN LEONESA CON LAS ENFERMEDADES DE LA SANGRE). León.
- ASCOL (ASOCIACIÓN CONTRA LA LEUCEMIA Y ENFERMEDADES DE LA SANGRE). Salamanca.
CATALUÑA
- ASSOCIACIÓ FÈNIX. Solsona
- FECEC (FEDERACIÓ CATALANA D’ENTITATS CONTRA EL CÁNCER
- FUNDACIÓ KÁLIDA. Barcelona
- FUNDACIÓ ROSES CONTRA EL CÀNCER. Roses
- LLIGA CONTRA EL CÀNCER COMARQUES DE TARRAGONA I TERRES DE L’EBRE. Tarragona
- MielomaCAT
- ONCOLLIGA BARCELONA. Barcelona
- ONCOLLIGA GIRONA. Girona
- ONCOLLIGA COMARQUES DE LLEIDA. Lleida
- ONCOVALLÈS. Vallès Oriental
- OSONA CONTRA EL CÀNCER. Osona
- SUPORT I COMPANYIA. Barcelona
- VILASSAR DE DALT CONTRA EL CÀNCER. Vilassar de Dalt
VALENCIAN COMMUNITY
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ASLEUVAL (ASOCIACIÓN DE PACIENTES DE LEUCEMIA, LINFOMA, MIELOMA Y OTRAS ENFERMEDADES DE LA SANGRE DE VALENCIA)
EXTREMADURA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- AFAL (AYUDA A FAMILIAS AFECTADAS DE LEUCEMIAS, LINFOMAS; MIELOMAS Y APLASIAS)
- AOEX (ASOCIACIÓN ONCOLÓGICA EXTREMEÑA)
GALICIA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- ASOTRAME (ASOCIACIÓN GALLEGA DE AFECTADOS POR TRASPLANTES MEDULARES)
BALEARIC ISLANDS
- ADAA (ASSOCIACIÓ D’AJUDA A L’ACOMPANYAMENT DEL MALALT DE LES ILLES BALEARS)
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
CANARY ISLANDS
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- AFOL (ASOCIACIÓN DE FAMILIAS ONCOHEMATOLÓGICAS DE LANZAROTE)
- FUNDACIÓN ALEJANDRO DA SILVA
LA RIOJA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
MADRID
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- AEAL (ASOCIACIÓN ESPAÑOLA DE LEUCEMIA Y LINFOMA)
- CRIS CONTRA EL CÁNCER
- FUNDACIÓN LEUCEMIA Y LINFOMA
MURCIA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
NAVARRA
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
BASQUE COUNTRY
- AECC (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER). Present is the different provinces and in many municipalities. Contact the nearest branch.
- PAUSOZ-PAUSO. Bilbao
AUTONOMOUS CITIES OF CEUTA AND MELILLA
- AECC CEUTA (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER)
- AECC MELILLA (ASOCIACIÓN ESPAÑOLA CONTRA EL CÁNCER)
Support and assistance
We also invite you to follow us through our main social media (Facebook, Twitter and Instagram) where we often share testimonies of overcoming this disease.
If you live in Spain, you can also contact us by sending an e-mail to imparables@fcarreras.es so that we can help you get in touch with other people who have overcome this disease.
* In accordance with Law 34/2002 on Information Society Services and Electronic Commerce (LSSICE), the Josep Carreras Leukemia Foundation informs that all medical information available on www.fcarreras.org has been reviewed and accredited by Dr. Enric Carreras Pons, Member No. 9438, Barcelona, Doctor in Medicine and Surgery, Specialist in Internal Medicine, Specialist in Hematology and Hemotherapy and Senior Consultant of the Foundation; and by Dr. Rocío Parody Porras, Member No. 35205, Barcelona, Doctor in Medicine and Surgery, Specialist in Hematology and Hemotherapy and attached to the Medical Directorate of the Registry of Bone Marrow Donors (REDMO) of the Foundation).
Become a member of the cure for leukaemia!


